Dry Eye Testing Options and What to Expect
Blog:Dry Eye Testing Options and What to Expect

Dry Eye Testing Options and What to Expect
If you frequently experience burning, redness, blurred vision, or a gritty sensation, you may be dealing with dry eye disease. At Texas State Optical Texas City, comprehensive dry eye testing helps identify the root cause of your symptoms so you can receive targeted, effective treatment.
Understanding Dry Eye Disease
Dry eye disease occurs when your eyes either don’t produce enough tears or produce poor-quality tears that evaporate too quickly. Healthy tears are made up of three layers - oil, water, and mucus - and each plays a critical role in keeping your eyes comfortable and your vision clear. An accurate diagnosis is essential because different types of dry eye require different treatment approaches. That’s why a thorough evaluation is the first step toward relief.
Comprehensive Eye Exam and Symptom Review
Your appointment will typically begin with a detailed discussion about your symptoms, lifestyle, medical history, and screen use habits. Certain medications, health conditions, and environmental factors can contribute to dry eye.
Your optometrist will perform a comprehensive eye exam to evaluate your overall eye health and rule out other conditions that may mimic dry eye symptoms. This foundational step ensures that nothing is overlooked.
Tear Film Evaluation
One of the most important aspects of dry eye testing is evaluating the tear film. Your doctor may use specialized diagnostic tools to assess how well your tears are functioning.
• Tear Break-Up Time (TBUT): This test measures how quickly your tears evaporate. A small amount of dye is placed in your eye, and your doctor observes how long it takes for dry spots to appear on the cornea. Rapid evaporation often indicates an unstable tear film.
• Tear Volume Testing: Tests such as the Schirmer test measure how much tear fluid your eyes produce over a specific period. This helps determine whether your dry eye is caused by insufficient tear production.
Meibomian Gland Evaluation
The meibomian glands in your eyelids produce the oil layer of your tears, which prevents evaporation. If these glands become blocked or dysfunctional, it can lead to evaporative dry eye.
Your doctor may gently examine your eyelids and use imaging technology to assess the structure and function of these glands. Identifying meibomian gland dysfunction (MGD) is critical because it’s one of the most common causes of dry eye.
Ocular Surface Staining
Special dyes may be applied to your eyes to highlight areas of irritation or damage on the cornea and conjunctiva. Under a blue light, these areas become more visible, allowing your optometrist to assess the severity of dryness and inflammation. This painless test provides valuable insight into how dry eye is affecting your eye health.
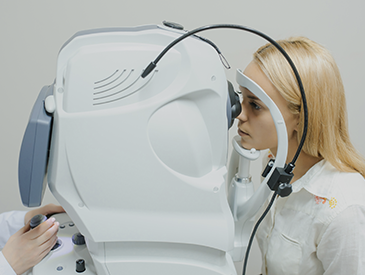
What to Expect During Your Appointment
Dry eye testing is generally quick, comfortable, and non-invasive. Most tests take only a few minutes and can be completed during a routine visit. You may experience mild temporary blurring from diagnostic dyes, but this typically resolves quickly.
After testing is complete, your optometrist will review the findings with you and discuss treatment options. Depending on the cause of your dry eye, recommendations may include prescription eye drops, eyelid treatments, lifestyle adjustments, nutritional supplements, or in-office procedures.
Get to the Root of Your Dry Eye Symptoms
Dry eye disease can impact your daily life, but the right testing and diagnosis can lead to meaningful, lasting relief. Advanced dry eye testing options help pinpoint the underlying cause of your symptoms so you can receive customized care designed for your specific needs.
If you’re experiencing burning, redness, fluctuating vision, or persistent irritation, don’t ignore the signs. Schedule a dry eye evaluation at Texas State Optical Texas City to find relief from dry eye symptoms and protect your long-term eye health. Visit our office in Texas City, Texas, or call (409) 202-6984 to book an appointment today.